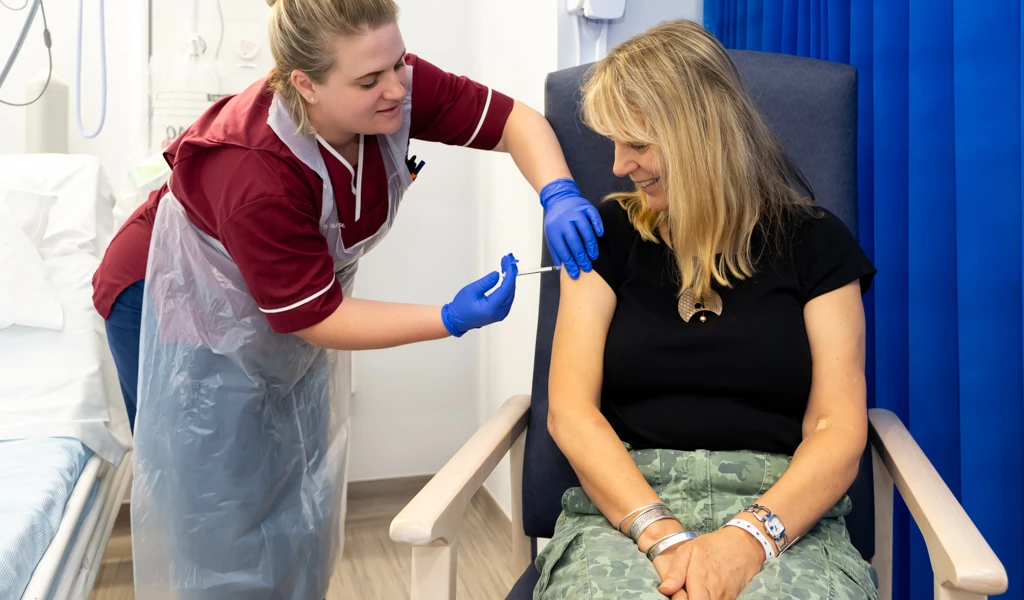
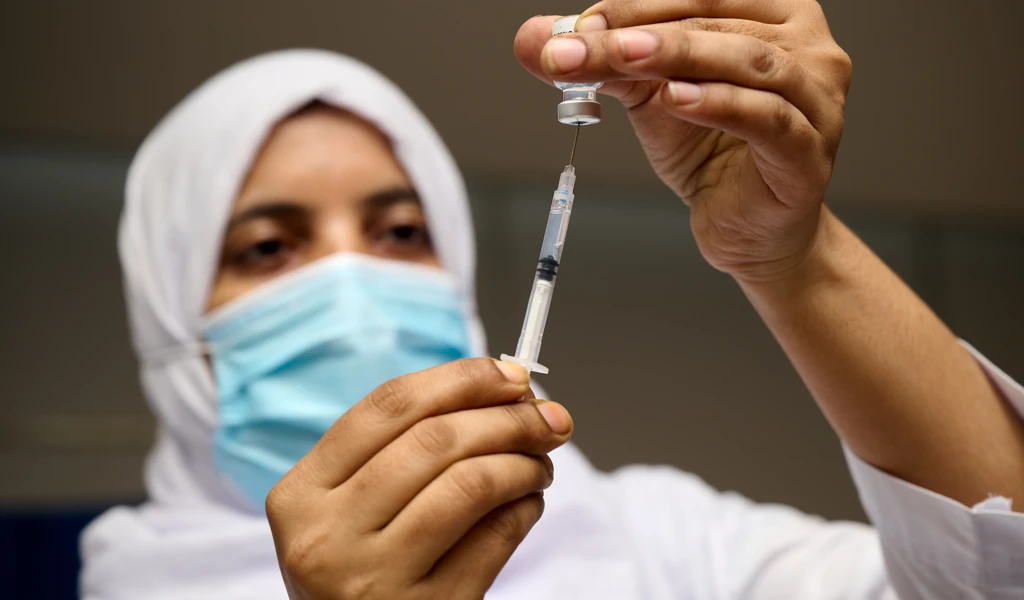
Climate change isn't just warming the planet, it's increasing spillover risks and pandemic threats

Our globally connected world has made us vulnerable to the rapid spread of new zoonoses—pathogens that jump from animals or birds into humans and cause outbreaks of disease. The emergence of another infectious disease with pandemic potential is inevitable. It's just a matter of time.
Climate change and environmental instability are expanding the range of disease-carrying animals such as mosquitoes and bats, which can migrate to and thrive in parts of the world where they were previously unable to survive. This in turn increases the number of animal-to-human interactions, boosting the chances that viruses and other pathogens might "spillover" from one species into another. With each spillover event comes a risk of a new human-adapted virus, or Disease X, emerging—just as SARS-CoV-2 did in late 2019.
As world leaders arrive at COP27 Climate Change Conference this week, CEPI caught up with Dr Aaron Bernstein, Director of the Center for Climate, Health, and the Environment at the Harvard T.H. Chan School of Public Health , to discuss with him how climate change is increasing pandemic risk and what he'd like to see world leaders do about it.
The interview has been edited for brevity and clarity.
Can you tell us briefly what your primary areas of research are?
I'm interested in the health effects of global environmental changes, such as climate change, and the loss of biological diversity, and especially how those things matter to health, and importantly, how the actions we can take to address those challenges can improve health, especially for at-risk populations.
What is a spillover event?
Spillover refers to the movement of a pathogen, which could be a virus or bacteria, parasites or really anything that can infect a person, from an animal to a person. That can occur from domesticated livestock like cows, chickens, or pigs, or it can occur from wild animals into people. Most spillover events do not cause disease in people. The pathogens may not, in fact, result in disease. But some do —and those are the ones we wind up reading about in the news.
And are such spillover events—the ones that do pose a problem for humans—a growing threat?
We know that, of the things that cause infectious diseases in people, about half, maybe even two thirds are pathogens that can infect other species. When you look at emerging infections -- these are new infections that we haven't heard of before, as well as diseases that are caused by resistant organisms—fully three quarters of those are the results of zoonotic diseases, ie, diseases that have spilled from animals into people. And of those emerging infectious diseases, the largest share is spillover from wildlife into people. Over the last several decades we're seeing more outbreaks from diseases spilling from animals into people.
It's very hard to cut down a lot of the world's forests, burn them down, and to mine into the recesses of the planets in places that are generally wild, and not have new opportunities for contact between people and animals.
What are the key risk factors then for those spillover events? Which of those risks are rising?
Spillover happens when people come into contact with animals, and we've been doing that at greater scale and in different ways over time. Certainly since humans have domesticated animals, we have seen spillover from livestock into people. And with huge livestock operations happening around the world in more places, there's more opportunity for pathogens to spill into people. We've seen that certainly with influenza pandemics, we saw it with the outbreak of Nipah virus in Malaysia, where bats infected domesticated pigs who spread it to people. There are lots of examples. But there are also increasing interfaces between humans and wildlife. It's very hard to cut down a lot of the world's forests, burn them down, and to mine into the recesses of the planet in places that are generally wild, and not have new opportunities for contact between people and animals. So those are some of the ways we are increasing risks of spillover.
And then there's climate change, which is forcing everything that can to get out of the heat. And that means running to the poles or up mountainsides - and animals in particular are bumping into each other in ways they didn't before. So, species that were geographically isolated, that didn't run into each other's paths, now, in fact are running into each other. We've seen evidence of this already with ungulates in Canada, where changing migration patterns has led to contact and the spread of disease among species. That's another source of increasing risk of spillover.
And if spillover is the spark that leads to outbreaks of disease, the lighter fluid on that spark is the dense human populations in cities, and air travel. There's no question that there is greater risk of disease spread when you have lots of people living in a relatively small place and lots of people travelling around the world and potentially spreading diseases quickly.

Rainforest destruction. Gold mining in Guyana, South America.
Is climate change simply expanding the geographical reach of animal vectors and hence increasing the number of people at risk?
We certainly have reason to believe that warming has made it possible for insects to live in places they've never lived before. We've seen that in United States with Lyme disease, which has now spread into Canada. There's good evidence that malaria in East Africa and in Andean countries in South America is able to do better at higher elevations because of warming. And there's a lot of evidence in diseases that affect animals—whether that's bird malaria in Hawaii, or other diseases—that these insects that transmit disease are living in places they couldn't live before and transmitting disease. So that is certainly one of the ways in which climate affects where diseases can happen. But I think it's important to remember that it is quite likely that in Western equatorial Africa, which is probably the place on Earth where malaria has been the longest and is most prevalent, it's going to get too hot. Most of the climate models suggests that we'll see less malaria in large parts of western Africa, because climate change will make it inhospitable to the disease.
There is no question that acting on climate change is a very wise decision if one is interested in limiting infectious disease spread of any kind.
So does a warming climate always only increase epidemic and pandemic risk? Or is there movement the other way: if places get too hot, then actually, the risk of epidemics of certain diseases or pandemics reduces in those areas?
I would say there are probably going to be some instances where climate change will make diseases less likely, and I think malaria in West Africa is probably one of the clear examples. But on the whole, there's no question that climate change is not good for infectious disease risk. Look, there's no malaria in the United States because of interventions that included draining wetlands, and using insecticides and using anti-malarial drugs, even as the climate warmed. Which is to say, most of the progress that we've seen in rolling back diseases, infectious diseases, has come from human interventions. Well, climate change really makes it hard to deliver health care. It interrupts supply chains. It destroys infrastructure, particularly water infrastructure, and certainly buildings through hurricanes, and a host of other effects, which will make—and already has made—containing infectious diseases harder.
One of the things history has taught us is that we can do reasonably well when we know the infectious diseases in a community and have tools to treat them, but when things are popping up where they are not expected, and where public health infrastructure is weakened, boy, that's when diseases really thrive. Another important factor is that climate change is forcing many, many people to move against their will. And those people are at very high risk of infectious disease outbreaks. That's another area in which we see infectious disease risk growing, even if it's, again, not about a specific vector or disease happening in a part of the world. It's just that those individuals often lack access to health care, they're often living in conditions where sanitation is difficult to maintain. So there is no question that acting on climate change is a very wise decision if one is interested in limiting infectious disease spread of any kind.
We have lots of evidence that we can stop spillovers. And the amazing part is that when you work upstream like this, you don't just prevent one disease, you prevent any disease. And oh, by the way, you save forest, which is a climate solution, you protect indigenous rights, which is a moral good, and, and a host of other benefits that you'll never ever get by trying to bring in a fire brigade after a disease appears.
There was some modelling that was published in Nature recently that showed that if even if global warming is held under the two degrees barrier within the 21st second century, that won't reduce viral spillover. So how are we going to cope in the near term? Is it all about improving surveillance so that we can spot these things quickly when they emerge?
That is one study, and I think it is a compelling study, but it is by no means the be all and end all of knowledge on this subject. There are a lot of things that they had to assume about how the world was going to work to get to the estimate that they made. And many of those assumptions may not hold up.
I think a lot is within our power to address emerging infectious disease risks. One of the things I've been talking about for a while is that we will never get ourselves out of emerging infectious disease risk through an after-the-fact-alone approach: that means waiting for diseases to appear in people, trying to detect them, and then trying to rush in and keep them from spreading. We'll always need to do that, diseases will always spill into people. But you know, if the last pandemic wasn't enough to show us that that approach doesn't make any sense, any pandemic prior to that would have made it even more painfully obvious that we really do need to focus on preventing spillover at the source. We can do that through conserving habitats, we can do that through improving biosecurity and livestock operations, we can do that through addressing risks in wildlife trade, and a host of other - what I would call - primary prevention activities.
Just to point out the absurdity of the bulk of the approach that has been directed towards addressing emerging infectious disease risks: we would never try and deal with climate change simply by building sea walls and desalinization plants and creating drought resistant crops. Because we know that we could never, frankly, do well as a civilization without addressing the root cause, which is mostly dealing with our addiction to fossil fuels. No one would say that's a wise approach, no one would say it makes any sense to simply try and adapt to this problem.
But that's really what we're doing here with emerging infections. We're essentially taking the stance that we're going to wait for these diseases to appear, try and catch them early, and hope that we have the resources and the governance structures to quench them. I think that is essential, but I also think we can do better. We have lots of evidence that we can stop spillovers. And the amazing part is that when you work upstream like this, you don't just prevent one disease, you prevent any disease. And oh, by the way, you save forests, which is a climate solution, and you protect indigenous rights, which is a moral good, and you get a host of other benefits that you'll never ever get by trying to bring in a fire brigade after a disease appears.

Pteropus bats, the natural hosts of Nipah virus.
Of the diseases that have already spilled over, things like Nipah, Rift Valley Fever, Chikungunya, and so on, which do you think is the most sensitive to a changing or warming climate?
There's no question in my mind the diseases that are transmitted by insects are very sensitive to warming climate, because the insects are limited in their range by temperatures. But also, we are seeing the pace of emerging infections growing, and we're not exactly eradicating these things, right? They're sticking around. So even with this idea of containment and preparedness, we are not able to eradicate diseases. We didn't eradicate HIV, we haven't eradicated dengue. It is extremely difficult to eradicate diseases once they've been in a population.
We did a study, published last year, where we looked at all of the emerging viral diseases that spilled into people from animals over the past century. And we found that every year, if you look at just the deaths from these pathogens, whether it's HIV or the pandemic flus or MERS or SARS, or you name it, we're losing hundreds of billions of dollars because they're all still around. In terms of where you throw money, it just doesn't make sense. You get so much benefit over the long-term from preventing these spillover events in the first place. And to your point, I don't know where climate change is necessarily going to hit the throttle on any of these diseases next, is very hard to know that. And so it's hard to make intelligent investments about what to do to prevent further spread in many cases. It just all comes back to the reality that we have an imbalance in our investments. We need to contain diseases that are already here. That's going to be an ongoing challenge. But, boy, haven't we learned enough to know that we need to prevent these things from happening in the first place? It seems to me that that couldn't be clearer.
We've got COP27 coming up this week, do you get a sense that there's enough focus at that Summit on the link between risk of climate change and pandemics?
There's some recognition, but it is siloed. I've been working on climate change and health for over 20 years and it took decades for people to acknowledge that climate change was a people problem. I think one might take a moment and reflect as to why it has been that way. How we can reconcile the reality that we have such amazing medical science—treatments, vaccines, tests, and so forth—and they're used to great benefit to society, and yet how difficult it has been to address the biodiversity crisis and climate. I think it's because the siloed approach, the reductionist approach, works extremely well if you take systems and make them very simple: like pathogens, there's one pathogen, there's one drug, there's one vaccine, and that's the whole problem. But it turns out that with those approaches, you don't in fact capture all the challenges you face: things like planetary-scale challenges, whether it's climate change or the biodiversity crisis. My hope is that we can increasingly point out that there is huge value—to governments and society—to multisolving here, to saying: wow, we could do something like conserve forests, we could get extra benefits from those investments for our climate goals, for our infectious disease goals, for our goals of conserving biodiversity, for our goals of protecting indigenous peoples' rights. That's what I'm hoping will come out of the pandemic. And my hope is that increasingly at places like COP27, and also at the meetings that are forthcoming around how we deal with pandemic, that our leaders and intelligent people will really be able to recognize this. There are serious headwinds. I'm not naive here. But the good news is that there's science and truth to what I'm saying that's hard to get around.
In the context of this conversation, is there anything else that you are worried about right now that you'd like to address?
Yes. I think there's a huge equity piece of this conversation that's important to air as well. So one other important point I'd like to make is that primary prevention [of spillover] is an inherently equitable approach to dealing with this, because the diseases are prevented in the places where they erupt. And those places are those which are often least equipped to do these things. Noteworthy is that in many low-income and middle-income countries, they have Ministries of One Health, and when you ask the folks running these ministries why they do, it's because they have to. They're never going to get past these challenges through technology alone. It's sort of obvious to them that this paradigm of ‘let's just come in and contain it' is foolish.
Watch the full interview with Dr Bernstein here.
Learn more about CEPI's spillover research here.